Telangana is overly focused on sterilisation. It needs to increase awareness about condoms, which only 0.8% men in the state use.
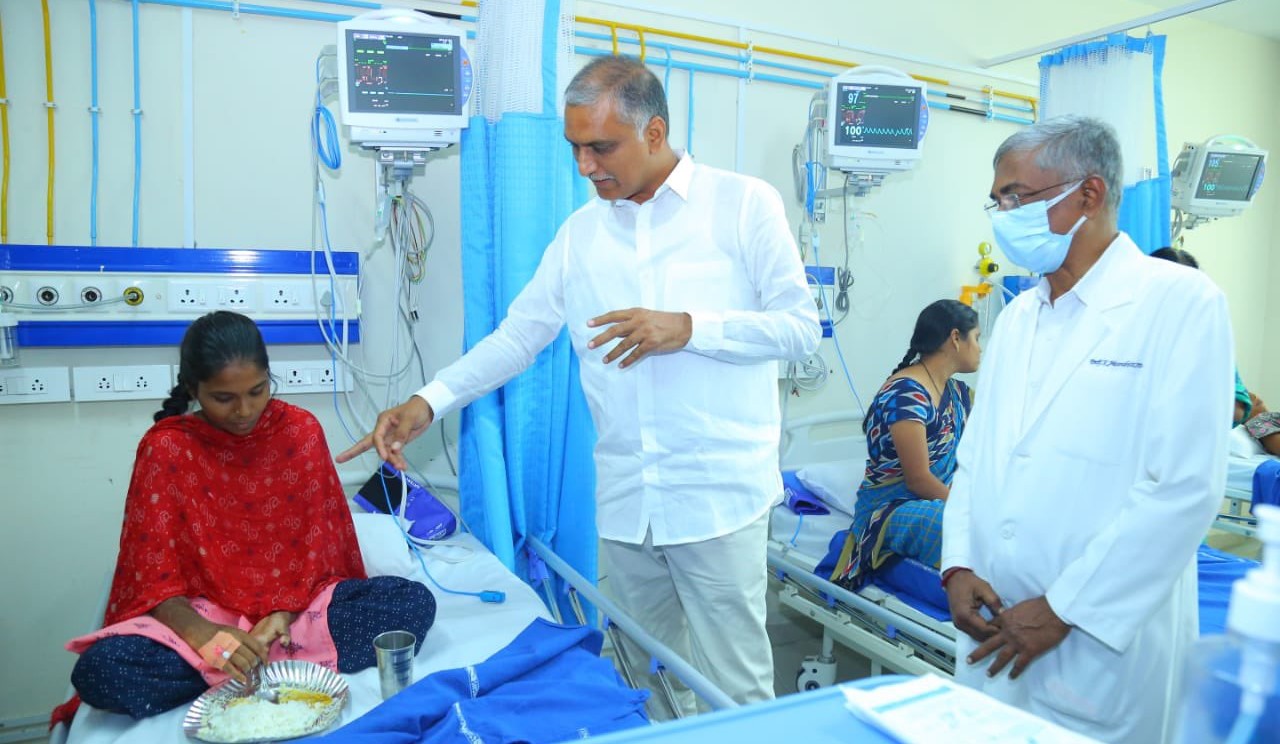
Telangana Health Minister T Harish Rao on Wednesday, 31 August, visited the NIMS Hospital to interact with some of the patients from the Ibrahimpatnam sterilisation camp where several women developed infections and four died (Twitter/@TelanganaHealth)
On 25 August, 34 women underwent Double Puncture Laparoscopy, a sterilisation method, at the Community Health Centre (CHC) in Ibrahimpatnam in Ranga Reddy district of Telangana. Within a few days, four have died while seven have suffered complications and are being monitored at a private hospital.
Sterilisation-related deaths aren’t new to India, where the quality of care often depends on where a public health facility is located and the socio-economic status of the people it serves.
In November 2014, 16 women died at a sterilisation camp in Bilaspur, Chhattisgarh, due to botched-up sterilisation surgeries. At the time, the Population Foundation of India led a fact-finding mission, resulting in a report titled ‘Robbed of choice and dignity: Indian women dead after mass sterilisation’.
The report recommended improving the quality of care by ensuring easy access to empanelled doctors, making appropriate information available in the local language, ensuring proper informed consent of the prospective patient, and diligent functioning of the Quality Assurance Committees at the state and district levels.
The report contributed to the landmark Supreme Court verdict in the Devika Biswas Vs Union of India case in 2016. The judgment laid the foundation for a rights-based approach to family planning and reproductive health by directing the state governments to stop the practice of holding sterilisation camps and fixing targets, and instead take measures to improve the overall quality of services.

One-year-old Karthik, whose mother is one of the 30 women who are hospitalised after they underwent surgery at the Ibrahimpatnam sterilisation camp (Sumit Jha/South First)
Yet many states continue to focus on female sterilisation, which has resulted in a skewed contraceptive method mix in the country. Female sterilisation contributes to the highest share of contraceptive usage in the country, placing the burden of family planning almost entirely on women.
Telangana’s current total fertility rate (TFR) is 1.75, according to the fifth round of the National Family Health Survey (2019–21). The state achieved the replacement level of fertility (TFR of 2.1 or less) in 2004 (then part of united Andhra Pradesh).
The modern contraceptive prevalence rate, or MCPR, stands at 66.7 percent and the total unmet need for family planning is reported at 6.4 percent in the state. However, the use of modern contraceptives is highly skewed towards female sterilisation, and it accounts for about 93 percent of total modern contraceptive use. Telangana reported the second-highest prevalence rate of female sterilisation in India during 2019–21 (61.9 percent), a few percentage points behind Andhra Pradesh (69.6 percent).
As per Census 2011, 29 percent of the state’s population is young (15–29 years). However, among young people, the unmet need for family planning, especially for spacing methods, is quite high (14.1 percent among those aged 15–19 years and 9.4 percent among those between 20 and 24).
On the other hand, the prevalence of modern methods of contraception is quite low among these age groups (6.4 percent among 15–19 years and 27.5 percent among 20–24 years). Thus, the need of the hour is to focus more on young people’s demand for spacing family planning methods.
The state is, however, still overly focused on sterilisation. Between April and July this year, the local health authorities in the state organised a total of 111 sterilisation camps and conducted 38,656 surgeries.
Telangana needs to focus on increasing awareness about, and access to, temporary contraceptives for young people, which include condoms, injectables, oral contraceptive pills, and emergency contraceptive pills.
Young people will be the largest cohort in the reproductive age bracket that will determine the population growth for the next couple of decades and it is imperative that they have regular access to a range of contraceptives of their choice.
Enhancing male engagement in family planning is imperative. In Telangana, only 0.8 percent of men use condoms and only 2 percent opt for vasectomies, according to NFHS-5.
The public health system primarily engages with women, rather than men. Thus, men do not generally participate in discussions about family planning and the burden of using contraception is primarily placed on women. According to a 2014 study, almost half of all Indian men (40.2 percent) — married or cohabitating — think it is a woman’s responsibility to avoid getting pregnant.
This needs to be addressed with focused social and behaviour change communication (SBCC) campaigns that challenge patriarchy and break regressive gender norms.
To avoid the recurrence of such tragedies, it is critical to maximise the reach and use of currently available choices by addressing issues including barriers related to access, fears, and misconceptions associated with contraceptive methods, providers’ bias, lack of awareness among clients and frontline health workers, geographical and economic challenges, and restrictive social-cultural norms.
(Poonam Muttreja is the executive director of the Population Foundation of India, and has for over 40 years been a strong advocate for women’s health, reproductive and sexual rights, and rural livelihoods. Before joining PFI, she served as the India Country Director of the John D and Catherine T MacArthur Foundation for 15 years and has also co-founded and led the Ashoka Foundation, Dastkar, and the Society for Rural, Urban and Tribal Initiative (SRUTI). These are the personal views of the author)

May 17, 2024

May 17, 2024

May 16, 2024

May 16, 2024

May 16, 2024

May 16, 2024