Published May 01, 2026 | 10:15 AM ⚊ Updated May 01, 2026 | 10:15 AM

KGMOA has sounded an urgent alarm, calling on the state government to confront the deep cracks in manpower and infrastructure.
Synopsis: The lack of proper treatment facilities and established guidelines has made it difficult for doctors in Kerala’s government hospitals to analyse and treat snakebite victims. Moreover, despite government directives that antivenom should be available at Community Health Centres and above, availability is inconsistent. Further, the lack of appropriate antivenom for some snakes in the Western Ghats complicates the situation.
Despite the rising number of snakebite cases and sightings across Kerala, a quiet crisis is unfolding inside hospital walls. In the dim hours of the night, when most snakebite victims are rushed into medical colleges, it is often young duty doctors who stand at the frontline — anxious, uncertain and burdened by the weight of decisions they are not fully equipped to make.
Fear is not just among the public; it lingers in emergency wards where every minute matters, yet clarity and support remain scarce.
The Kerala Government Medical Officers Association (KGMOA) sounded an urgent alarm, calling on the state government to confront the deep cracks in manpower and infrastructure. While proposals to expand treatment facilities offer some hope, doctors warn that the reality on the ground is far more fragile.
Also Read: Your guide to the snakes behind Kerala’s fatal bites
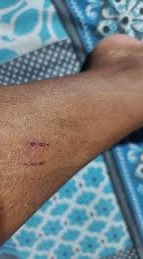
Doctors are often forced to write ”insect bite” or ”query(?) snakebite” if there are no clear bite marks.
When South First spoke with several young doctors working in district hospitals and medical colleges, many of whom highlighted the difficulty in confidently confirming snakebite cases. In most emergencies, doctors cannot wait for blood test confirmation and must rely entirely on clinical suspicion.
Dr Sunil PK, President of the KGMOA, explained that when preparing case summaries, doctors are often forced to write ”insect bite” or ”query(?) snakebite” if there are no clear bite marks. In many cases, identifying the bite itself is difficult — sometimes only a single mark is visible, making confirmation even harder.
To determine envenomation, doctors depend on neurological assessment and proceed with Anti-Snake Venom (ASV) based on suspicion.
Dr Sunil stated that administering ASV carries a significant risk of anaphylaxis, a severe and potentially life-threatening allergic reaction, with a probability of around 30–43 percent.
He also highlighted the pressure surrounding referrals, stating that if a doctor refers a patient and the condition worsens during transfer, the consequences can be serious, and the responsibility ultimately falls on the doctor.
“Doctors in Kerala have differing opinions in treating snakebites,” said Muhammed Anwar Yunus, Biodiversity Cell Chief of the Kerala Forest Department and SARPA State Nodal Officer, speaking to South First.
He pointed out that even basic first-response measures remain debated. Also, there are conflicting views on whether ASV should be administered in every suspected case. Some doctors support immediate administration, while others consider it risky.
”Kerala does not have a detailed, uniform protocol for snakebite treatment — that is a reality. Although snakebite has now been included as a notifiable disease following a suo motu case by the Kerala High Court and despite a 2024 circular from the Union Health Ministry directing states to notify snakebite cases, gaps remain in clinical clarity,” he said.
The National Action Plan for Prevention and Control of Snakebite Envenoming (NAPSE), launched in March 2024, aims to reduce snakebite deaths by 50 percent by 2030. However, Yunus noted that Kerala has gone a step further, formulating its own state-level action plan to eliminate snakebite deaths by 2029.
Yet, he stressed that institutions such as the National Centre for Disease Control (NCDC) and the Indian Medical Association (IMA) still lack detailed guidance on crucial aspects such as when exactly to administer ASV, at what intervals and in which cases it can be avoided.
“Even manufacturers admit that existing antivenoms are not effective in all cases,” he added.
Also Read: Kerala finally declares snakebite a notifiable disease
Despite government directives that antivenom should be available at Community Health Centres and above, the reality on the ground is starkly different.
“In Kerala, antivenom is mostly available only at taluk-level hospitals and above, and even there, availability is inconsistent,” Yunus pointed out.
This creates dangerous delays. Doctors, he added, often hesitate to administer ASV due to the absence of a uniform protocol and fear of complications.
Echoing this concern, Dr Sunil told South First, “After administering ASV, close monitoring is essential. The patient must be observed every five minutes. But doctors are simultaneously handling OP duties, dog bite cases, medico-legal work such as drunkenness certification and accident cases. How can they provide such intensive care?”
”If we refer a patient and their condition worsens during transfer, who takes responsibility? When patients are brought unconscious, snakebite is often not suspected immediately. Now, we are planning to train doctors in view of the unusual surge in cases.” he said.
To address infrastructure gaps, discussions are underway for public-private partnerships.
“We are planning coordination between private and government hospitals for snakebite management. Private hospitals have better ICU and ventilation facilities, and the government can bear the expenses,” he added.

hump-nosed pit viper
Apart from protocol confusion, Kerala faces a critical medical limitation — the lack of effective antivenom for several local snake species. Currently, hospitals rely on polyvalent antivenom sourced from Tamil Nadu, designed to treat the “big four” snakes — Indian cobra, Russell’s viper, common krait, and saw-scaled viper.
However, officials acknowledge that this antivenom is ineffective against many species found in the Western Ghats.
A major concern is the hump-nosed pit viper, responsible for hundreds of cases annually. Kerala records around 3,500–4,500 snakebite cases each year, with about 30 percent involving venomous snakes. Of these, roughly 335 cases are attributed to hump-nosed pit viper bites.
Other species lacking effective antivenom include the Malabar pit viper, bamboo pit viper, large-scaled pit viper and even the king cobra.
To address this gap, the state is planning to develop region-specific antivenom at the Kerala State Drugs and Pharmaceuticals Ltd. in Alappuzha and potential collaborations with established manufacturers.

Uthra
Yunus also highlighted the forensic and legal challenges associated with snakebite deaths, citing the well-known Uthra case. The case involved a 25-year-old woman who was killed by a snakebite while asleep on 7 May 2020. Investigators had to prove that the bite was planned by her husband and not accidental.
“I was part of the team. Forensic experts struggled to collect evidence. In court, only evidence matters; we had to prove it was a forced bite, with close proximity, multiple bites and induced action, not a natural incident.”
The Kerala Police even sent the snake carcass for DNA analysis. The cobra, about 80 cm long, was capable of delivering a fatal bite. The then-DGP Loknath Behra confirmed that the investigation would proceed scientifically.
“It was extremely complicated. We could not get every detail, even during the postmortem examination,” Yunus noted.
This case underscores the legal vulnerability doctors face. Without clear protocols, they risk scrutiny and liability in complex cases.
“Doctors should be given legal protection to save them from future consequences,” he stressed.
According to the Ministry of Health and Family Welfare’s Standard Treatment Guidelines (2017), snakebite management is a time-critical emergency. For a doctor, a snakebite is a race against time- where every decision can save a life. But in that race, who protects the one making those decisions?
(Edited by Muhammed Fazil.)

