Published Jul 29, 2024 | 7:00 AM ⚊ Updated Jul 29, 2024 | 7:00 AM
Facva, a five-year-old girl who was undergoing treatment at the Government Medical College Hospital in Kozhikode, Kerala, for primary amoebic meningoencephalitis (PAM), passed away on 20 May. She was the first of three in Kerala who died due to PAM this year.
The other two, EP Mridul (12) from Kozhikode, and V Dakshina (13) from Kannur, are the other two who succumbed to the infection.
While these cases are sporadic, in a rare instance this year, a 13-year-old boy from Melady in Kozhikode has recovered.
According to the state’s health department, PAM has been reported in many parts of Kerala over the last decade. As of 7 July this year, five cases of PAM have been reported from North Kerala.
“Clinical features were suggestive of PAM. The cases over the last two months have been reported in children aged 5, 13, 12, 13, and 15 years, with a male-to-female ratio of 3:2,” stated the state guideline.
The Union government has now released a report detailing the microbial features of the amoeba. Of the five cases, clinical reports suggest that Vermamoeba vermiformis is the major amoeba for the infections and subsequent deaths.
“Out of the five cases, three have microbiological features of Vermamoeba vermiformis and one case has been confirmed as Naegleria fowleri through PCR testing,” the Union Health Ministry stated in parliament. However, researchers believe that Vermamoeba vermiformis is not responsible for PAM.
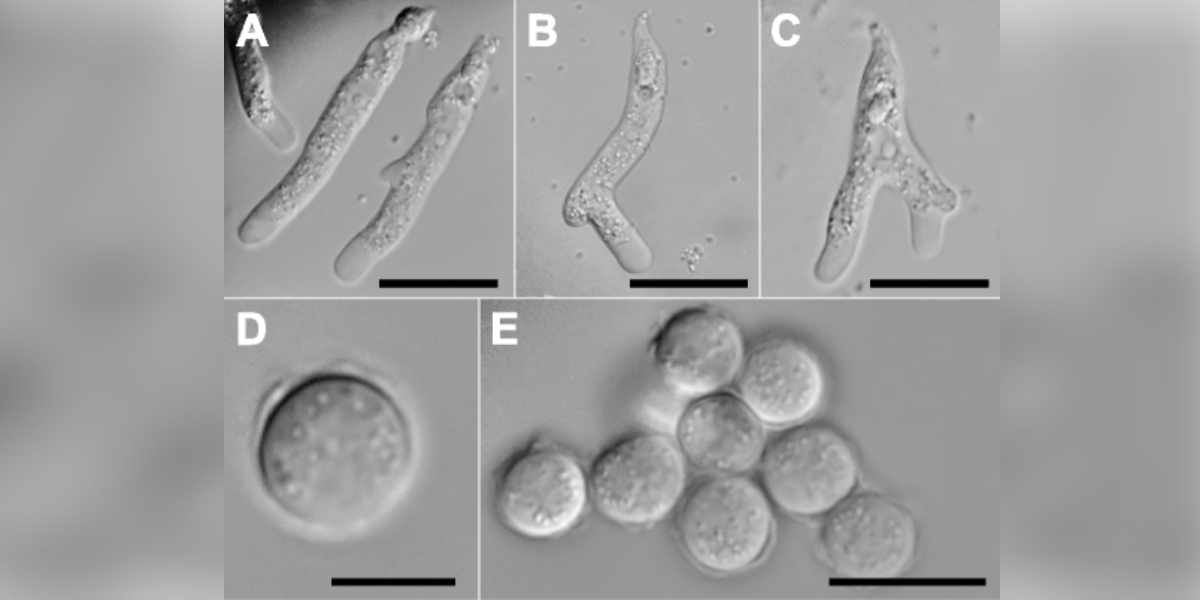
Vermamoeba vermiformis is a free-living amoeba commonly found in soil and freshwater environments. It is known for its amoeboid movement and ability to form cysts. While generally not pathogenic to humans, it is significant due to its presence in environments where other pathogenic amoebae, such as Naegleria fowleri, are found.
Vermamoeba vermiformis is not responsible for PAM; that role is specifically attributed to Naegleria fowleri. However, the former can be associated with other infections and is considered a potential reservoir for pathogenic bacteria, which can complicate clinical outcomes in immunocompromised individuals.
Both V. vermiformis and Naegleria fowleri are found in similar warm and freshwater environments. This overlap raises concerns about the potential for co-infection or the presence of multiple pathogenic organisms in the same habitat, posing risks to human health.
Species-Specific Pathogenicity: PAM is specifically caused by Naegleria fowleri, a free-living amoeba that infects humans by entering through the nasal passage, traveling along the olfactory nerves, and reaching the brain. Naegleria fowleri has specialised mechanisms to breach the blood-brain barrier and cause inflammation and destruction of brain tissue.
Invasive Behaviour: Naegleria fowleri is thermophilic, thriving in warm freshwater, and has a particular invasive behavior that allows it to penetrate the nasal mucosa and migrate to the brain. Vermamoeba vermiformis does not exhibit this invasive behaviour and lacks the ability to migrate through the nasal passage to the brain.
Trophozoite Stage: The trophozoite stage – activated, growing or vegetative stage in the life cycle of the specific parasite – of Naegleria fowleri is highly aggressive and can directly invade human tissue. Vermamoeba vermiformis does not have such an invasive trophozoite stage capable of causing significant human tissue damage.
Virulence Factors: Naegleria fowleri produces specific virulence factors, including amoebic proteases, that enable it to break down host tissues and evade the immune system. Vermamoeba vermiformis lacks these specific virulence factors and associated pathogenic mechanisms.
While Vermamoeba vermiformis is not directly pathogenic to humans in the context of PAM, it remains relevant in microbial ecology due to its interactions with other microorganisms, potentially affecting their survival and virulence.
PAM is a rare but severe infection of the central nervous system caused by the free-living amoeba Naegleria fowleri. This organism is typically found in warm freshwater environments, such as lakes, rivers, hot springs, and poorly maintained swimming pools. Infection occurs when contaminated water enters the body through the nose, usually during water-related activities like swimming or diving.
Symptoms
Symptoms of PAM typically appear within 1 to 12 days after exposure to contaminated water, with an average onset around five days. Initial symptoms resemble those of bacterial meningitis and may include:
– Headache
– High fever
– Nausea and vomiting
– Stiff neck
– Confusion and hallucinations
– Seizures
As the disease progresses, it can lead to severe neurological impairment and death, often within 1 to 2 weeks of symptom onset.
Diagnosis
Diagnosing PAM can be challenging due to its rapid progression and similarity to other forms of meningitis. Common diagnostic methods include:
– Lumbar puncture (spinal tap) to analyse cerebrospinal fluid (CSF) for the presence of amoebas.
– Imaging tests (CT or MRI) to rule out other conditions.
– Specialised laboratory tests, such as PCR, to detect the genetic material of Naegleria fowleri in CSF or brain tissue samples.
Treatment
There is no standard treatment for PAM, and the prognosis is generally poor, with a fatality rate exceeding 98 percent. However, some studies suggest that a combination of antifungal and antiamoebic medications, such as miltefosine, amphotericin B, and fluconazole, may improve outcomes if administered early.
Prevention
Preventive measures include avoiding warm freshwater environments, using nose clips while swimming, and ensuring proper chlorination of swimming pools. Education about the risks associated with water activities in warm conditions is crucial, especially for children and young adults, who are more commonly affected.
The infection was first detected in the state in 2016 and has recurred in various districts, including Malappuram, Kozhikode, and Thrissur, with the latest incidents occurring in northern Kerala. The Ministry stated that diagnostic testing results for five children with a clinical diagnosis of Acute Encephalitis and cerebrospinal fluid (CSF) shows motile amoeba.
– In 2016, the first confirmed PAM case was reported in Alappuzha district.
– Between 2019 and 2020, cases were reported in Malappuram district.
– In 2020, cases were reported in Kozhikode district.
– In 2022, cases were reported in Thrissur district.
– In 2023, cases were again reported in Alappuzha district.
(Edited by Neena)
(South First is now on WhatsApp and Telegram)

