Published Sep 26, 2024 | 7:00 AM ⚊ Updated Sep 26, 2024 | 7:58 PM
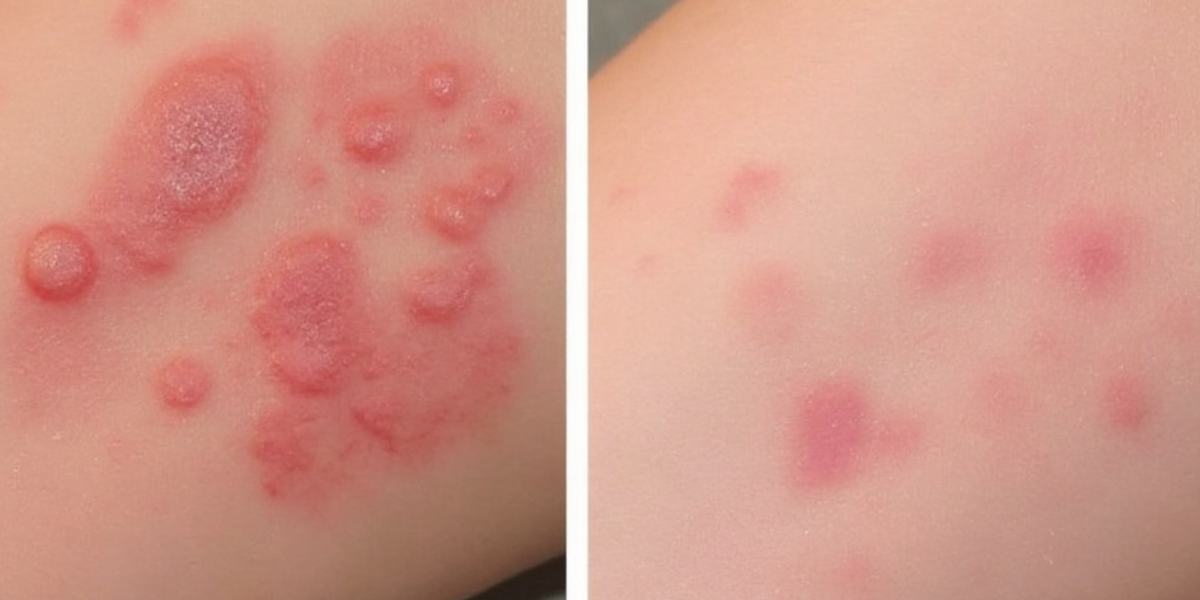
How to differentiate between Mpox and Chickenpox?
As India reports its first case of the virulent clade 1b strain of Mpox in Kerala, many travellers returning from abroad are becoming anxious about symptoms of illness, wondering if these are related to Mpox.
Several viral diseases share common symptoms with Mpox. Chickenpox is the disease that is most similar in its presentation.
Understanding these differences is crucial for accurate diagnosis and treatment. While both Mpox and chickenpox can present with similar initial symptoms — such as fever and rash — lesion size, pain level, distribution, and duration are different and can help tell the difference between the two infections.
Initial symptoms
Differences in rashes
Pain vs itchiness
Lymphadenopathy
Swollen lymph nodes are more frequently observed in cases of Mpox compared to chickenpox.
Duration of symptoms
Mpox symptoms can last longer than chickenpox symptoms, often extending up to four weeks.
Mpox (which used to be called monkeypox) shares symptoms with several other diseases, which can complicate diagnosis.
Smallpox
Syphilis
Herpes Simplex Virus (HSV)
HIV/AIDS
Shingles (Herpes Zoster)
Zika virus
The case was identified in a 38-year-old man from Malappuram district who had recently returned from the United Arab Emirates. He is currently stable and receiving treatment at a government medical college hospital in Kerala.
In response to this case, Kerala health authorities have ramped up surveillance and monitoring efforts. They are tracking over 70 individuals who were in close contact with the patient, including 29 friends and family members and 37 fellow airline passengers, all of whom have shown no symptoms so far. Isolation facilities have been established across the state, and additional testing centers are being considered to manage potential cases.
While health officials indicate that the likelihood of a large-scale outbreak remains low, they continue to monitor the situation closely.
Various state governments have prepared hospitals with isolation wards and enhanced surveillance at points of entry into the country. Public health campaigns are also being promoted to raise awareness about prevention and hygiene practices related to Mpox.
Clade 1b is considered more virulent compared to other strains and has been linked to outbreaks primarily through sexual contact. This strain was first detected in the Democratic Republic of the Congo earlier this year and has since spread to several countries, including Sweden and Thailand, making India the third country outside Africa to report it.
The World Health Organisation (WHO) declared Mpox a Public Health Emergency of International Concern (PHEIC) in August 2024 due to the rapid spread of this strain.
There are two distinct clades of the virus: clade I (with subclades Ia and Ib) and clade II (with subclades IIa and IIb).
Clade 1b is a new offshoot of clade I that has been spreading person-to-person in the Democratic Republic of the Congo (DRC) since 2022.
“Clade 1b is new, and genetic analysis indicates that this virus jumped from forest animals to humans as recently as September 2023. Since then, Clade 1b has spread mostly within the DRC and to neighbouring countries in Africa. Outside of Africa, one travel-related case each has been detected in Sweden and Thailand. The WHO issued the PHEIC early so that other nations could also prepare, monitor for cases, and send samples for sequencing to better understand how Clade 1b behaves outside of Africa,” Chairman of Indian Medical Association Research Cell Kerala State Dr Rajeev Jayadevan told South First.
Studies have shown that clade I infections, including clade 1b, are linked to increased rash intensity and higher viral loads compared to clade II. This may facilitate transmission through close contact and skin-to-skin contact during sexual activity.
The WHO Director-General stated that the emergence of clade 1b in the Democratic Republic of the Congo (DRC) and its detection in neighbouring countries is “especially concerning” as it is spreading “mainly through sexual networks.” In a 2024 outbreak in the Kamituga mining region, 88 percent of hospitalised cases reported transactional sex, demonstrating how sexual networks can facilitate transmission.
Also, the emergence of clade 1b has been associated with shifts in transmission dynamics, particularly through sexual contact. Recent studies indicate that clusters of transmission linked to heterosexual and same-sex intimate contact have become more prevalent, which was not as commonly observed in previous outbreaks. This change suggests that sexual networks are now significant contributors to the spread of Clade 1b.
While monkeypox is typically a zoonotic disease with limited person-to-person spread, the unexpected global outbreak of the clade IIb virus in 2022 suggested the virus may be adapting to a new host – humans. The emergence of clade 1b with increased transmissibility indicates further adaptation.
Higher viral load in clade 1b
Clade 1b infections are associated with greater disease severity, including more pronounced rashes and higher viral loads compared to other clades. This increased severity can enhance the likelihood of transmission through direct contact with lesions or bodily fluids. Evidence suggests that rash intensity and detectable viral loads are greater for clade 1 than for clade II, facilitating more efficient spread during close contact situations.
“When we see reports indicating that many infected individuals are children, we must consider this in context. As for transmission, we know that Mpox spreads through substantial physical or sexual contact. Whether respiratory droplets play a role is still uncertain, though it’s possible they could play a role during very close contact. However, it likely won’t spread from casual encounters, such as sharing a bus ride or classroom with an infected person. This remains an area of uncertainty, so we need to monitor it closely. The spread and severity of cases reported in central Africa could be influenced by the general health status of the population, the congested living conditions in some strife-ridden areas, and the availability of healthcare locally,” said Dr Jayadevan.
The Mpox outbreak has disproportionately affected the LGBTQIA+ community, particularly men who have sex with men (MSM), leading to increased stigma and discrimination against this group. This situation has been exacerbated by societal perceptions and media narratives that frame Mpox as a “gay disease,” which can perpetuate harmful stereotypes and discrimination.
The framing of Mpox within the context of LGBTQIA identities has led to a resurgence of anti-LGBTQIA rhetoric. This has manifested in online platforms, where individuals have been blamed for the spread of the virus, reinforcing negative stereotypes about promiscuity and moral character among gay and bisexual men.
The stigma surrounding Mpox can deter individuals from seeking medical attention or disclosing symptoms due to fear of discrimination. This reluctance can ultimately hinder public health efforts to control the outbreak, as people may avoid testing or treatment, leading to further transmission of the virus.
(Edited by Rosamma Thomas)

