Published Apr 12, 2023 | 9:00 AM ⚊ Updated Apr 12, 2023 | 9:00 AM

Dr Narendra Gupta and his team have been fighting hard against unnecessary hysterectomies since 2013. (Creative Commons)
Meet the man whose public interest litigation (PIL) against the rampant practice of “unnecessary hysterectomies” in India has led the Supreme Court to recently direct all states and Union Territories (UTs) in India to implement guidelines formulated by the Centre to check the menace.
Dr Narendra Gupta from Rajasthan is a physician and public health expert who has been advocating against unnecessary hysterectomies, especially of poor women, where the purpose is to rake in high insurance fees from governments under various health insurance schemes.
Speaking to South First, Dr Gupta said that he and his team have been fighting hard against unnecessary hysterectomies since 2013 and, finally, 10 years later, the Supreme Court has made a positive move.
“In many countries, hysterectomy is typically conducted amongst pre-menopausal women above the age of 50 years. In India, we have been seeing, despite several efforts, high hysterectomy rates amongst young women, ranging from 28-40 years of age,” he said.
Dr Gupta is the founder of the non-profit organisation Jan Swasthya Sahyog (JSS), which provides medical care and advocacy for marginalised communities in rural India.
A hysterectomy is a surgical procedure that involves the removal of a woman’s uterus, which is often done to treat various health conditions such as uterine fibroids, endometriosis, and cancer.
However, statistics from surveys done across the country, have shown that a large number of unnecessary hysterectomies are being performed, especially among women under 40 years of age.
This has raised serious concerns about the physical, emotional, and social consequences of the procedure, and the need for strict guidelines to be put in place.
Dr Gupta explained to South First that, in 2013, they found that in districts of Rajasthan, a large number of women were subjected to hysterectomies and this was done in a very hush-hush manner, mostly in private hospitals.
“They were taken to private hospitals, an ultrasound was done, and they were advised removal of their uterus, stating that their problems of painful menstrual cycles, heavy bleeding would stop if they had this surgery. A majority of the women were 27-28 years of age,” Dr Gupta explained.
He said that these women, if they had children, would be told that the job of uterus is over and they don’t need one any more. When the numbers went up, a local organisation picked up this issue and contacted Dr Gupta and asked him to investigate.
“I did some fact-finding and found the allegations to be true. We then approached the Human Rights Law Network in Delhi, which is an organisation of lawyers. Together, we decided to file a PIL. We also did a consultation with gynaecologists and other stakeholders,” Dr Gupta explained.
He said that a letter was written to the then health secretary in 2014, asking them to include a section on the rate of hysterectomies in the country, which was added to the National Family Health Survey (NFHS-4).
Despite a series of scandals related to unnecessary hysterectomies in not just Rajasthan being reported, the frequent use of hysterectomies continues in young women.
With an intention to put a stop to this and to make states, districts, as well as private and government hospitals accountable for this, a PIL was filed by Dr Narendra.
The NFHS of women aged 15-49 years indicated that approximately 1 in 10 women in India would have undergone a hysterectomy by age 50.
NFHS-4 (2014-15) and NFHS-5 (2019-21) reported similar prevalence, indicating no substantial reduction in hysterectomies over the past 10 years. Interestingly, as per the NFHS data, the highest rate of hysterectomies were reported in Andhra Pradesh, Telangana, Bihar, and Gujarat in the last 10 years.
“Amongst the southern states, in Andhra Pradesh and Telangana, over 20 percent of women in the age group of 40-49 years have already had a hysterectomy. The highest prevalence is in rural areas,” Dr Gupta explained.
Also, the Central government has taken note that since the launch of Ayushman Bharat PM-Jan Arogya Yojana in 2018, nearly 45,434 hospital admissions — worth ₹126 crore — has been authorised under it for hysterectomy-related treatment.
Ayushman Bharat PM-Jan Arogya Yojana is the world’s largest publicly-funded health assurance scheme, providing health cover of ₹5 lakh per family to 12 crore families.
Dr Gupta cited statistics that nearly two-thirds of the total hysterectomy cases — about 33,559 procedures — were conducted in private hospitals and only 11,875 were done in government hospitals.
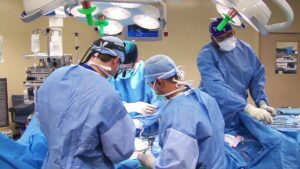
Majority of hysterectomies in the country are allegedly happening at private hospitals. (Wikimedia Commons)
He said that while Uttar Pradesh conducted the highest hysterectomy procedures conducted in private hospitals at 10,341, southern state Kerala followed with 7,549 procedures, Gujarat with 6,605, Haryana with 5,034, Madhya Pradesh with 2,913, Andhra Pradesh with 2,525, and Uttarakhand with 2,042.
The Supreme Court also directed the states to introduce open audits and clinical governance within facilities to review and monitor hysterectomy cases, especially when recommended for younger women in both private and government facilities.
However, Dr Prakash Kini, obsterician at Cloud Nine Hospitals, whom South First spoke to, said, “It is irrelevant to audit a private set-up as most patients are educated but such an audit is definitely relevant to do in government hospitals.”
However, the Supreme Court said that all states and UTs in the next three months should adopt the guidelines issued by the Ministry of Health and Family Welfare mentioned in the status report. And the court hopes that the real picture will emerge after the data is made available.
The apex court permitted the Centre to take necessary policy decisions once every six months.
The leading causes of a hysterectomy reported by women are gynaecological symptoms, such as excessive menstrual bleeding and pain.
The availability of gynaecological services in primary and secondary care, uneven distribution of gynaecologists, and varying capacity to address women’s reproductive health are also few health system factors influencing hysterectomy numbers.
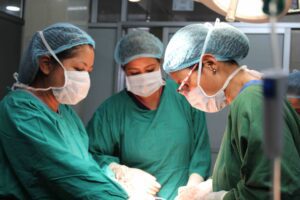
Hysterectomy is being touted as a ‘permanent solution’ to gynaecological problems. (Wikimedia Commons)
“In India, the median age of a hysterectomy is at least a decade earlier than natural menopause when compared to other high-income countries. The numbers are high among rural, uneducated women for a complex web of reasons, including exploitation by private doctors, pressure from contractors, and difficult health and living conditions. Unfortunately, a hysterectomy at a young age is touted as a ‘permanent solution’ to gynaecological problems, like irregular bleeding, fibroids, and even lack of health care,” said Dr Gupta.
The response report submitted by the stakeholders to the court also states, though the role of health insurance in exacerbating the use of hysterectomy remains unclear, it is a critical issue to address.
“Hysterectomy claims under national schemes have been concentrated in six states, including Karnataka,” it noted. The other states on the list include Chhattisgarh, Uttar Pradesh, Jharkhand, Gujarat, and Maharashtra.
Dr Gupta pointed out that the practice of early and often unnecessary hysterectomy will have higher risk factors for chronic diseases, which are the leading cause of mortality amongst women in India.
There have been studies indicating increase in risk of osteoporosis or weakening of bones and cardiovascular diseases amongst women who have undergone hysterectomy.
Also, oophorectomy, the removal of ovaries, which is frequently done along with hysterectomy can also lead to decrease in hormone levels and lead to surgical menopause.

