Published Mar 24, 2025 | 7:00 AM ⚊ Updated Mar 24, 2025 | 7:00 AM
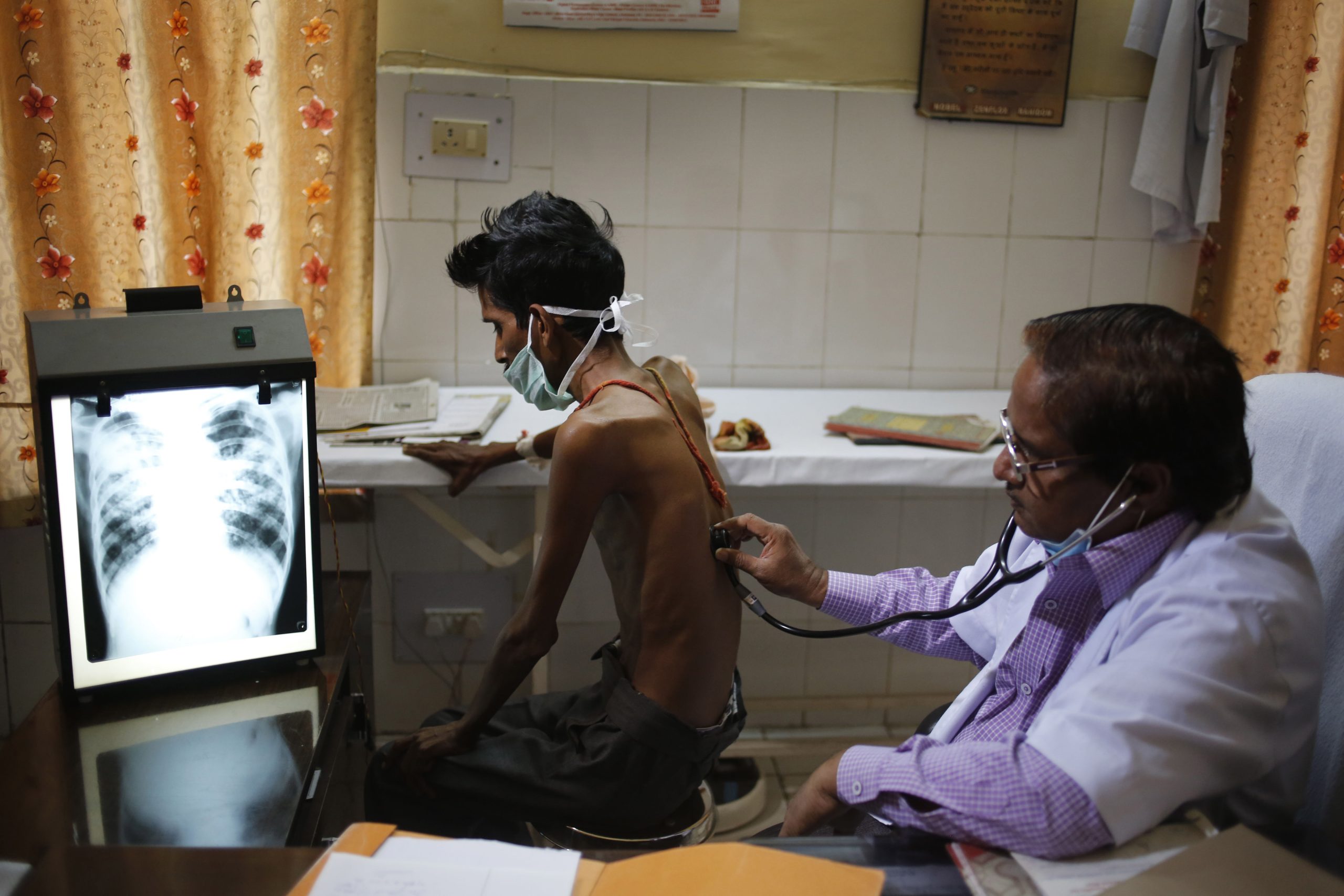
A doctor examining a tuberculosis patient at a TB hospital in India. (WHO website)
Synopsis: On World Tuberculosis (TB) Day, India reported 5,77,712 TB cases in just 81 days of 2025, highlighting the ongoing health challenge. Malnutrition, which weakens immunity and lung defences, is a major factor in TB’s spread. Dr. A Rajashyam, Telangana State TB officer, emphasised that undernutrition increases susceptibility to severe TB and can lead to Nutritionally Acquired Immunodeficiency Syndrome (N-AIDS)
Imagine your body is like a cricket team, and your immune system is the team’s defence—bowlers, fielders, and strategists—working together to stop the opposing team, which in this case is Tuberculosis (TB).
To win a match, the team needs good players, strong stamina, and proper training, just like your body needs nutrition to stay strong and fight off diseases.
Now, imagine if the team doesn’t get proper food, water, or rest. The players become weak, tired, and slow, struggling to bowl, field, or chase the ball. This is what happens when someone is undernourished—their immune system becomes weak, making it easier for TB to attack. But TB is not just any opponent—it’s a ruthless one that doesn’t just score runs; it also takes away the energy of your best players.
“TB and undernutrition are closely linked in a two-way cycle, where TB causes severe weight loss, and undernutrition increases the risk of TB infection. When TB bacteria infect a person, the immune system releases cytokines to fight the disease. However, these cytokines also increase metabolism and break down fat and muscle, leading to rapid weight loss, a condition known as cachexia,” said Hyderabad based pulmonologist Dr M Rajeev to South First.
On other hand, when TB infects someone, it causes loss of appetite and weight, making the body weaker and unable to fight back. It’s like the opponent stealing your best batsmen and bowlers mid-match, leaving your team with fewer resources to win.
“TB disrupts hunger signals in the brain, causing loss of appetite, while fever and night sweats increase energy expenditure, further depleting the body’s nutritional reserves,” said Dr Rajeev.
He added that TB also damages the digestive system, making it harder for the body to absorb essential nutrients. “As a result, TB patients often experience severe malnutrition, weakness, and delayed recovery, creating a downward spiral where poor nutrition weakens the immune system further, allowing TB to become more aggressive,” he said.
He pointed out that just like no cricket team can win a match with only good strategies but weak players, no TB patient can recover with only medicine but no proper nutrition. A player needs both batting skills and strong muscles to hit sixes, just like a TB patient needs both medicine and food to fight the infection effectively.
“The first few months of TB treatment are like the powerplay overs—the most critical period. If the body gets enough food and energy during this phase, it can fight TB more effectively, reduce the risk of complications, and ensure a full recovery,” said Dr Rajeev.
With World Tuberculosis (TB) Day, observed on 24 March, India already reported 5,77,712 TB cases within the first 81 days of 2025, according to the Ni-Kshay portal, highlighting the ongoing public health challenge posed by the disease. In India, which accounts for one in four cases of TB globally, according to a report by the World Health Organisation (WHO), nutrition becomes the core of the treatment of this disease.
“Being undernourished makes a person more likely to develop TB in the first place. The immune system requires proteins, vitamins, and minerals to effectively fight infections, but malnutrition weakens white blood cells, reducing the body’s ability to resist TB bacteria. Vitamin and mineral deficiencies lower lung defences, allowing TB bacteria to thrive. Severely malnourished individuals (BMI <14 kg/m²) develop Nutritionally Acquired Immunodeficiency Syndrome (N-AIDS), which significantly increases their risk of severe TB infection,” said Dr. A Rajashyam Telangana State TB officer to South First.
He pointed that studies show that undernourished individuals are 3-4 times more likely to develop TB than those with proper nutrition.
To break this cycle, TB patients must receive adequate nutritional support along with medication. Providing high-calorie, protein-rich foods, micronutrient supplements, and financial support can help patients regain weight, recover faster, and reduce the chances of relapse. At the same time, improving nutrition in vulnerable communities can help prevent TB infections before they occur, strengthening India’s fight against the disease.
Even studies in India suggest that if a TB patient is provided with better nutrition, it can turn around the outcome.
The RATIONS trial in Jharkhand, India, published in The Lancet Global Health, provides compelling evidence that undernutrition is a leading risk factor for TB mortality, treatment failure, and relapse. Undernutrition is not only a consequence of TB but also a major cause of disease progression. The study found that 82 percent of TB patients were underweight (BMI <18.5 kg/m²), and 17.3 percent had severe undernutrition (BMI <14 kg/m²).
The nutritional deficiency is associated with poor treatment adherence, delayed recovery, and increased risks of relapse and death. Moreover, severely malnourished patients are at higher risk of drug toxicity, anaemia, and infections, further compromising their ability to recover.
It emphasises that nutritional interventions must be considered an essential component of TB care, rather than just an auxiliary support measure.
So, the study tested the effects of nutritional support in TB patients by providing food rations (1,200 kcal and 52g of protein daily) and micronutrient supplements for up to 12 months, depending on disease severity. The results showed remarkable improvements: 93.7 percent of patients successfully completed treatment, significantly improving survival rates. Patients gained an average of 4.6 kg over six months, and weight gain in the first two months reduced mortality risk by 61 percent.
“Our results show a predictive effect for undernutrition at enrolment, and a protective effect of weight gain for tuberculosis mortality,” said the authors of the study.
Another recent Lancet Global Health Report (2025) presents a comprehensive roadmap for integrating nutritional assessment, counselling, and support into TB care.
The paper suggests that at treatment initiation, TB patients should undergo BMI measurement, mid-upper arm circumference checks, and haemoglobin testing to assess malnutrition and anaemia.
Since anaemia affects up to 94 percent of TB patients, routine haemoglobin screening is crucial. Early nutritional support, including protein-rich diets and food supplementation, can significantly reduce mortality. Household contacts of TB patients should also receive nutritional support, as studies indicate a 40 percent lower TB risk among well-nourished families.
It further suggests at the end of treatment, undernourished patients require close monitoring to prevent relapse. Governments must link TB survivors to welfare programs to prevent food insecurity. The report calls for mandatory nutritional data reporting, integration of nutrition into national TB strategies, and global funding for TB nutrition programs.
The report concludes that nutrition is as essential as antibiotics in TB treatment, urging immediate action to ensure better treatment outcomes, reduced mortality, and TB elimination.
In October, the Union Health Minister JP Nadda, announced that the government has approved an additional allocation of ₹ 1,040 crore for nutritional support for tuberculosis (TB) patients under the Ni-Kshay Poshan Yojana (NPY).
In an official statement, the Ministry of Health and Family Welfare said that it has decided to increase the monthly nutritional support under NPY to ₹1,000 per patient from the existing ₹500.
The government has also decided to permit expansion of the scope and coverage of the Ni-Kshay Mitra initiative under the Pradhan Mantri TB Mukt Bharat Abhiyan (PMTBMBA) to include the family members (household contacts) of TB patients.
“The government has also decided to introduce energy dense nutrition supplementation for all patients with BMI<18.5 and to permit expansion of scope & coverage of Ni-Kshay Mitra initiative under Pradhan Mantri TB Mukt Bharat Abhiyaan (PMTBMBA) to the family members (household contacts) of TB patients,” he said.
(Edited by Ananya Rao)

